Comprehensive care for bone fractures and trauma injuries using advanced techniques for optimal healing and recovery. From diagnosis to rehabilitation, we provide complete fracture management solutions.
If you suspect a fracture, don't wait! Immediate medical attention is crucial for proper healing and to prevent complications.
Expert management for all types of bone fractures and trauma injuries

A clean break where the bone breaks but does not pierce the skin. These are the most common types of fractures.

The broken bone pierces through the skin, creating an open wound. These require immediate surgical intervention.

The bone shatters into three or more pieces. These complex fractures often result from high-impact trauma.
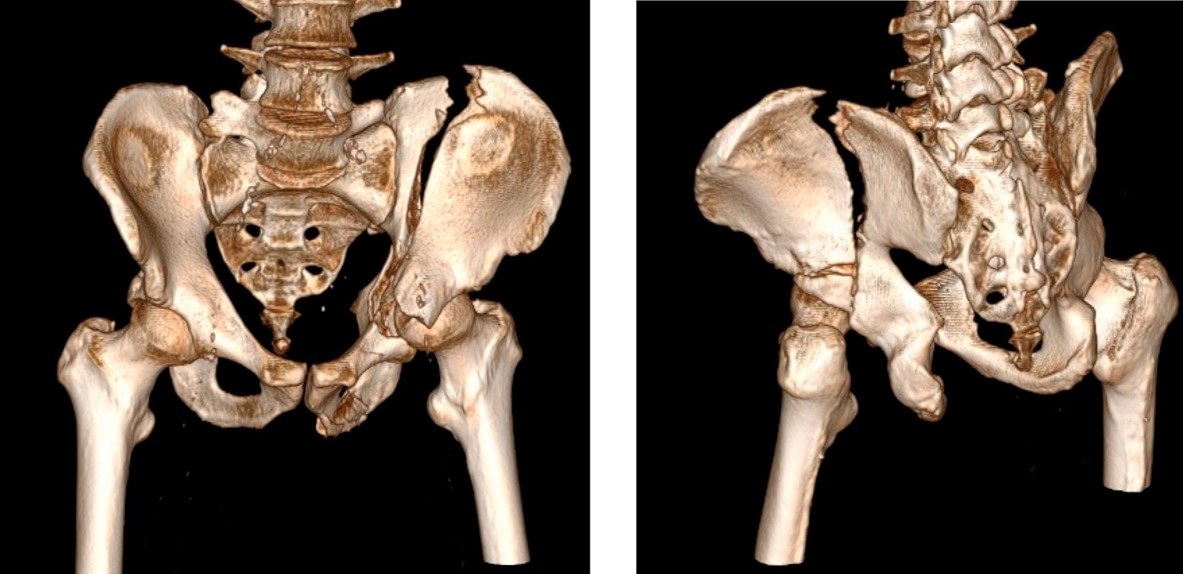
High-energy trauma fractures involving the pelvic ring or the acetabulum (hip socket). Frequently associated with life-threatening bleeding, visceral injuries, and long-term complications such as avascular necrosis or post-traumatic arthritis. Require specialized surgical reconstruction and multidisciplinary management.
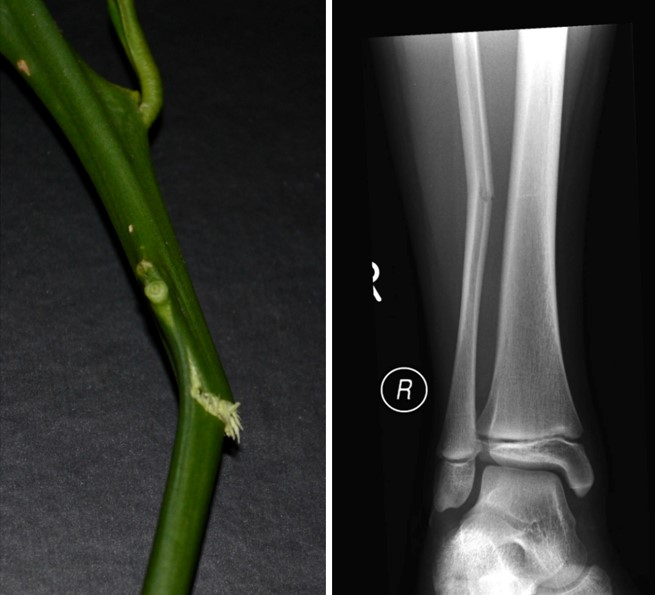
Common in children, where the bone bends and cracks but doesn't break completely, similar to a green twig.
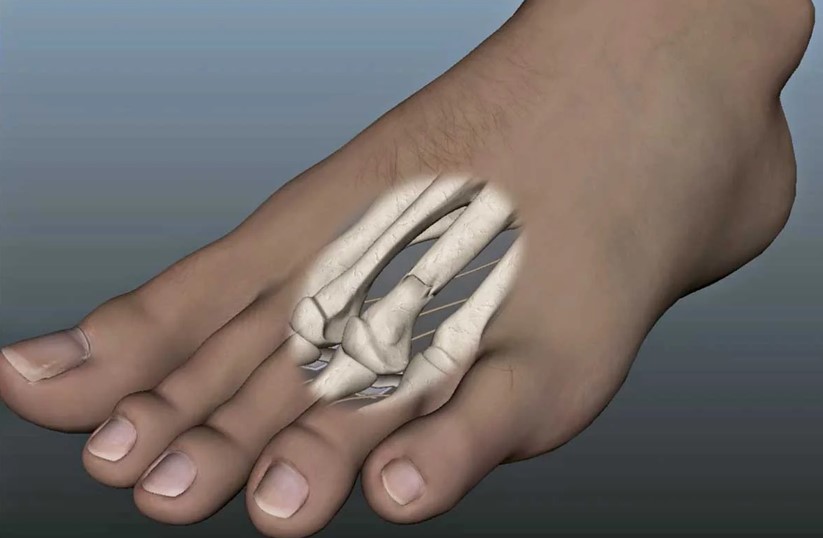
Small cracks in the bone caused by repetitive force or overuse, common in athletes and military recruits.
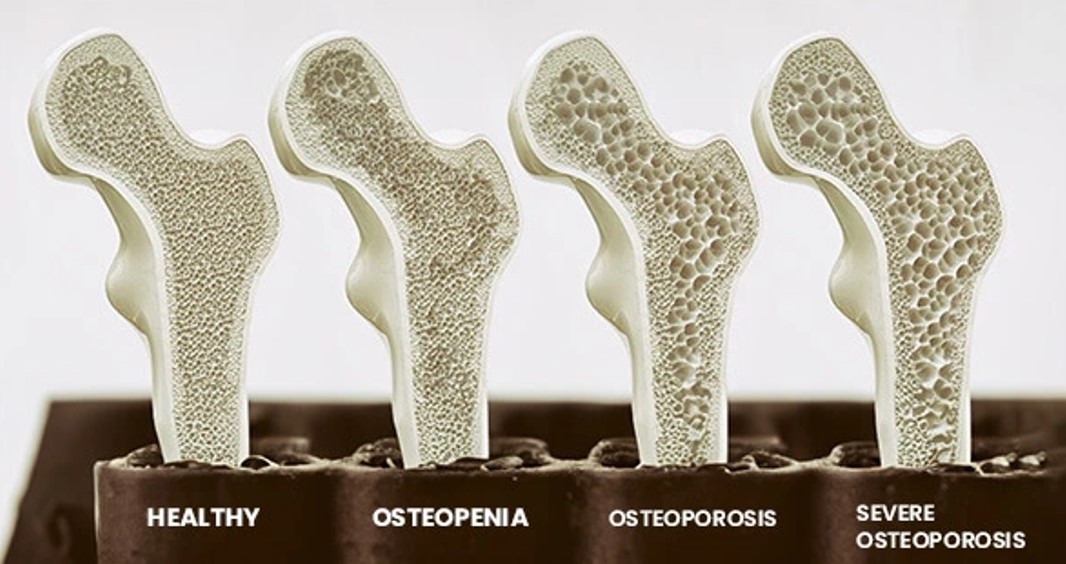
Fracture occurring in bone weakened by an underlying disease (osteoporosis, bone tumors, metastases, osteomyelitis, Paget's disease, etc.). Minimal or no trauma needed. Treatment focuses on both fracture stabilization and addressing the primary bone pathology.
State-of-the-art techniques for optimal fracture healing and recovery
Traditional plaster or fiberglass casts to immobilize the fracture and allow natural bone healing. Used for stable, non-displaced fractures.
Removable or adjustable supports that provide stability while allowing some movement. Ideal for minor fractures or during later healing stages.
Specialized braces that allow controlled movement while providing support. Promotes healing while maintaining joint function.
Application of a pulling force to align bone fragments. Used for certain types of fractures before definitive treatment.
Plates, screws, rods, or pins are surgically implanted to hold bone fragments in place. Allows early mobilization in many cases.
Metal pins or screws inserted into the bone above and below the fracture, connected to an external frame. Used for severe open fractures.
A metal rod is inserted into the marrow canal of long bones to stabilize the fracture. Minimally invasive with small incisions.
Transplanting bone tissue to help fractured bones heal. Used when there is bone loss or poor healing potential.
Structured exercises to restore strength, flexibility, and range of motion after fracture healing. Essential for full recovery.
Gradual increase in weight-bearing activities based on fracture healing stage. Monitored by orthopedic specialists.
Focuses on restoring ability to perform daily activities and return to work. Particularly important for upper extremity fractures.
Comprehensive approach to managing pain during recovery, including medications, modalities, and alternative therapies.
Step-by-step journey from injury to full recovery
Immediately after the fracture, the body initiates an inflammatory response. Blood vessels at the fracture site rupture, forming a hematoma (blood clot). This phase includes swelling, pain, and initial stabilization of the fracture.
Soft callus formation begins as fibroblasts produce collagen to form fibrocartilage. This is gradually replaced by a hard callus as osteoblasts create new bone. The fracture becomes stabilized by this new bone formation.
The hard callus is remodeled into compact bone along stress lines. Excess bone is resorbed, and the bone gradually returns to its original shape and strength. This phase can continue for up to two years after the fracture.
Complete restoration of function and strength. Implementation of strategies to prevent future fractures, especially for those with osteoporosis or other risk factors.
Understanding risks and how to prevent them
While most fractures heal well, potential complications can include:
Reduce your risk of fractures with these strategies:
Common questions about fracture management and recovery
While both can cause pain and swelling, fractures typically have more specific signs: inability to bear weight, deformity or abnormal positioning of the limb, bone protruding through skin (open fracture), grating sensation or sound during movement, and severe pain that doesn't improve with rest. However, only an X-ray can definitively diagnose a fracture. If you're unsure, it's always best to seek medical evaluation.
Healing time varies depending on several factors: the bone involved (small bones heal faster), fracture type and severity, age (children heal faster), overall health, and nutrition. Generally, most fractures take 6-8 weeks for initial healing, but complete remodeling can take up to 12-18 months. For example, a simple wrist fracture may heal in 6 weeks, while a tibia (shin bone) fracture may take 3-6 months or longer.
This depends on the specific fracture, treatment method, and your overall health. With surgical fixation using rods or plates, you may be allowed partial weight-bearing within days to weeks. With conservative treatment in a cast, non-weight-bearing may be required for 6-8 weeks. Your orthopedic surgeon will provide a specific timeline based on follow-up X-rays showing healing progress. Physical therapy plays a crucial role in safely returning to walking.
Nutrition is crucial for bone healing. Focus on: Calcium-rich foods (dairy products, leafy greens, fortified foods), Vitamin D (sunlight, fatty fish, eggs, fortified foods) for calcium absorption, Protein (lean meats, fish, eggs, legumes) for collagen formation, Vitamin C (citrus fruits, berries, peppers) for collagen synthesis, Zinc and Magnesium (nuts, seeds, whole grains) for bone metabolism, and adequate hydration. Avoid excessive alcohol and smoking, which impair healing.
Contact your doctor immediately if you experience: increased pain despite elevation and pain medication, numbness or tingling in fingers/toes, pale or blue discoloration of skin beyond the cast, inability to move fingers/toes, foul odor from the cast, cracking or softening of the cast, or if the cast feels too tight after swelling has subsided. These could indicate complications like compartment syndrome, infection, or circulation problems.
In most cases, yes. After immobilization, muscles weaken, joints stiffen, and proprioception (joint position sense) decreases. Physical therapy helps restore strength, flexibility, balance, and function. The duration and intensity depend on the fracture location, severity, and your goals. For simple fractures, a few weeks may suffice; for complex fractures or athletes returning to sports, several months of therapy may be needed. Early, appropriate rehabilitation significantly improves outcomes.
Whether you have an acute fracture or a healing concern, our orthopedic specialists provide comprehensive fracture management using the latest techniques. From emergency care to rehabilitation, we're here to guide you through every step of recovery.